“MemSaab, my neighbor’s wife is very sick,” began the village headman in slow, formal Nepali. “Do you have any medicine that would help her?”
It was 1978. I was traveling on foot with a small team of local staff in a rural district of Nepal, conducting an immunization campaign and providing simple health teaching in remote villages. A newly-minted nurse practitioner, I also tried to help villagers who came to me with their health problems. Two months after signing on, I was learning to cope with the major challenges of learning a new language, making long treks on difficult terrain, and persuading mothers with fears about immunizations to surrender their children to western medicine.
The village headman who was asking for my help was a tall, solemn-looking man wearing western clothes, as most of the village leaders did. At his side was his neighbor, a disheveled-looking man in his late forties, dressed in typical village attire. He shifted restlessly, a look of shock mixed with fear in his eyes.
After a few questions, I realized the problem was likely a serious one, and the three of us set off for the man’s house. On the way, I learned that his wife, Maya, was 28 years old and they had no children. Was she pregnant? He hesitated. Yes, maybe, he said. She had gotten a tetanus shot from our team during a previous visit to Borlang some two months prior. Not long after, she thought she was pregnant, attributing it to the “medicine.” Then, early this morning, she had sudden abdominal pain, so severe she could barely speak, and was getting weaker all the time.
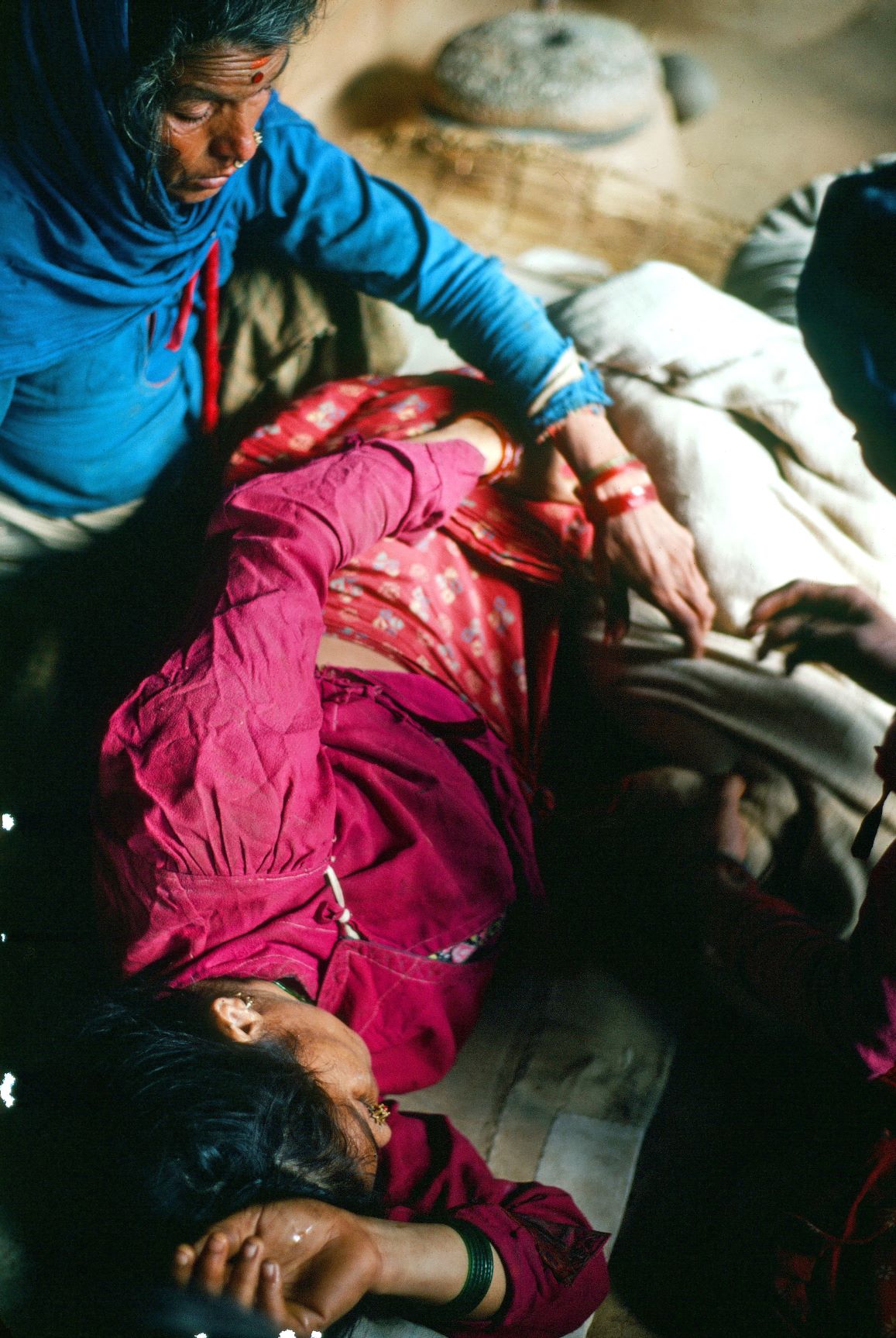
I followed the chief and his neighbor a short distance from our camp to a small thatched-roof house, where a very pale woman lay in the shade on the open porch. Several village women huddled around her, holding her hands, trying to comfort her. As I knelt down beside her on the straw mat, they moved aside. Maya’s lips and ears had a milky pale sheen and she was damp with perspiration, moaning and whispering words I couldn’t understand.
“Maya,” I asked gently, taking her hand. “Kosto chhah? Kahaa dukhyo?” How are you? Where does it hurt? She pointed weakly at her abdomen, and her arm dropped back to her side. I slid my hand gently under her wrinkled cotton cummerbund and felt a rigid, board-like abdomen underneath. A bad sign. Her pulse was a very rapid, thready tapping that told me she was going into shock.
“Dheri dukhyo,” an older woman said, looking at me with sad, questioning eyes. She hurts a lot. I nodded and felt a surge of sympathy not only for Maya, but also for the whole group of concerned friends and relatives. The sour scent of anxiety, of fear, filled the air around us. They were sharing her suffering, just as I was. The difference was that I was also expected to do something to help.
I considered the most likely causes of Maya’s condition. At the top of the list was a ruptured ectopic pregnancy, a serious complication where the embryo settles in the one of the fallopian tubes instead of the uterus. As it grows, it bursts the thin tube walls. Even if that wasn’t the cause, something bad had happened internally and, if she could be saved, it would require surgery very quickly.
“Ke garne?”What to do? That question, posed by the village chief, was on everyone’s mind. I looked around at the gathered villagers, who eyed me expectantly, as if waiting for my proclamation.
I knew there were only two realistic choices. They could transport Maya to the district’s Protestant mission hospital, around an eight-hour walk away. It was a well-run hospital with basic surgical capacity, something the government hospital, which was a mere four hours away, didn’t have. If she arrived in time and if the surgeon was there, an operation could save her life. The other choice: bring on the traditional healer, gather the family, say prayers, make offerings, and when she died, mourn yet another maternal death. The futility of either option weighed on me.
Everyone stood as if on alert, waiting for my advice.
I’d worked for several years in an emergency room in the U.S., so dealing with sudden, life-threatening crises wasn’t new to me. Once, when I was the evening triage nurse, a woman was brought in with similar symptoms. Within minutes of the diagnosis of an ectopic pregnancy, she was prepped for surgery and sent off for what turned out to be a fairly routine operation. The transfusion of a pint or two of blood, a couple of days in the hospital, and she was home again, sad at losing her pregnancy, but physically intact. That was the option that I wanted for this lovely young woman. Maybe it was possible.
Maya’s husband looked at me expectantly, and we stepped away from the main group of onlookers to speak in low tones.
“Sir, your wife is very sick,” I explained to him, swallowing between sentences. “She may die if she doesn’t have an operation.” I said I thought that Maya was bleeding inside, and the only treatment would be for her to have surgery to stop the bleeding. If they could get her to the local mission hospital, maybe she could be saved. Maybe, I repeated several times–as if this could absolve me of guilt if the plan failed.
Maya’s husband looked at me, seemingly bewildered at this information. A lengthy discussion with the chief and neighborhood men ensued. She was so sick, could the doctor really help her? Wasn’t there something else that could be done? But after much debate, they agreed to transport her to the hospital.
The first plan was to load her sitting upright into a dhoko, the cone-shaped basket that was used for hauling most goods on the area’s rocky trails, and that was often used to transport sick people. I quickly explained that no, she needed to lie flat, so her blood could circulate to her head; that would require making a stretcher. More discussion. How many men would it take to carry her on a stretcher? How would they make the device? Who could spare the day or two it would take for them to be away from their work?
As the men negotiated, I knelt by Maya to check her pulse and try to reassure her.
“We’re taking you to the hospital, Maya,” I said, leaning close to be sure she could hear me. I hoped that if she were alert enough to understand, she would find comfort in that plan. However, I also knew that “hospital” was a last resort for many village Nepalis, undertaken rarely and only when other options had been exhausted. She didn’t respond and perhaps didn’t even register what I was saying.
For the next two hours, I circled the throng, trying to understand what was being done and why it was taking so long. Why is nothing happening? Don’t they get it? The burden of her care seemed to rest on my shoulders, and it was heavy. I was the nurse in charge, just as I had been in that emergency room back home. It was my responsibility to see that things were done quickly, efficiently. But I’d never been faced with this kind of challenge. There was no backup plan, no on-call doctor, no surgical team, no emergency supplies. And no chaplain to call on when everything else failed.
Finally, the crowd moved aside as Maya’s husband and another man approached the house with a cleverly contrived stretcher of rope and wooden poles.
“Ah, that’s good,” I said. They laid the stretcher on a flat spot on the ground some distance from the porch and placed a heavy blanket on top. Uh-oh, I thought, panic rising in my throat. They want to carry her over to the stretcher like a sack of rice. Carrying her any distance would be painful and might also make the internal bleeding worse.
“You need to put the stretcher right next to her on the porch,” I advised. They nodded, and the neighbors moved back as the stretcher was positioned beside Maya. I helped the men lift her, straw mat and all, directly onto the device.
Maya moaned as she was settled onto the stretcher. Her husband leaned over and spoke to her softly, and she gave an even softer moan in response. When he stood back up, his face was grave, but had a new look of determination. An older woman from the gathering stepped back up to whisper something to her, and everyone moved off the porch to give the men room.
Three volunteers would help the woman’s husband carry the stretcher. They took their positions, one at each corner and, after a few false starts, hoisted it up and moved into the sunlight. Maya cried out briefly as the men shifted her position to even the load, startling the crowd. The older woman, who by now I realized was Maya’s mother, stepped up to give her daughter’s hand a farewell touch. Her face was a study in grief.
At last the four men began the long trek down the path and out of sight. Gradually the gathered villagers drifted away, with somber looks and muttered conversations. I began taking deep, slow breaths, trying to release the tension that had been growing all that afternoon.
An unsettling realization surfaced that had been nagging at me. As close as I was growing to my Nepali friends on the team, if it had been any of them who had gotten so ill, the scant possibilities for treatment would have been just the same as Maya’s. Back then, emergency care options for rural Nepalis were essentially nonexistent. Yet, if it was I who had fallen off a cliff or had a sudden attack of appendicitis, there would have been an immediate effort to get word to our office in Kathmandu, and a medical helicopter dispatched to fly me to care. The chasm between me and them was enormous. Maya showed me the stark face of the extent of my privilege, and it was deeply disturbing. Even though now, some forty years later, health services are much more widely available in Nepal, the gap between the care available in rural and urban areas is still substantial.
By the time Maya’s entourage had left, most of my health team had arrived to see what was happening, and we started a slow march back to camp. One of the vaccinators, Sita, asked me with a questioning frown what had happened, what had made the woman so sick.
I explained the basic information about an ectopic pregnancy. “No one really knows why this problem happens,” I said. Her puzzled look didn’t disappear.
Then she said gently, “You know, the neighbors are worried that someone put an evil spell on her.”
I gave myself a mental smack on the forehead. Of course. Though I’d often heard Nepali beliefs about the supernatural causes of illness, I’d once more forgotten that perspective and reverted to my biomedical thinking. They had been skeptical about what “modern” medicine could do for this problem, thus the lengthy discussions about how to respond. Why go to the hospital when Western doctors don’t know how to treat supernatural problems? They were probably also doubtful about going because good care was so rarely available in the rural clinics.
Yet, somehow, my advice to transport Maya had prevailed. My burden felt even heavier, and I held on ever more tightly to hope that she would survive. Will they make it on time? I asked myself for the rest of that afternoon, over and over. Was it the right decision to advise them to go? If she dies–will the tetanus shot be blamed, as immunizations sometimes are when unusual problems followed the injection?
Gathered on mats in a dark room near the cooking fire, we had an uneasy supper. The flickering flames reflected somber, thoughtful faces. The team’s usual joking and chatter were sparse now, and I imagined they were all wondering: What happened to Maya? When will we know?
After the meal, as we were about to move into the next room to prepare for tomorrow’s work, I heard an unfamiliar male voice conversing with a porter just outside. Sita stepped out to join them and returned moments later with a solemn expression, a little frown and half-closed eyes. She glanced around the room, waiting for silence.
“She died, about halfway to the hospital. They’ve come back,” was all Sita said.
Murmurs of dismay and sympathy rippled through the room. I felt a sudden thud in my chest: my fears were confirmed. A confusing mix of sadness and self-doubt settled on my shoulders, covering me like a dark cloud. Was it a mistake to send her off like that? Poor Maya had died in such pain, and I could do so little to help her or her distressed husband.
I took a deep breath and said, “Oh, Sita, how sad. But we did all we could. It was just too late.” I wanted to comfort the team, but there was little comfort for any of us in those words. I turned and made my way slowly to my tent, the last ounce of energy draining from my limbs.
Years later I still wonder if, knowing what I do now, I should have done anything differently on that afternoon in Borlang. In a career spent working in women’s health in many different international settings, nothing has had as profound an impact on how I view the world as seeing Maya being carried away, in a futile effort to avert her death.
Maya’s fate embodies that of so many women living in poverty, for whom just getting pregnant is a mortal risk. And it’s not only a problem in the poorer regions of the world. Disturbing reports have recently emerged about a rise in deaths in the U.S. due to pregnancy, which were already far higher than in the other industrialized countries. Black women in particular are much more likely to die from a problem related to childbearing than other groups.
When a pregnancy goes wrong, full access to quality care is often the only way to prevent the death of that mother-to-be. I learned that lesson long ago in Nepal. We need to learn it again today.
[Editor’s Note: This article rightfully stresses the importance of universal quality healthcare and an end to poverty, both in the U.S. and around the world, to help prevent unnecessary deaths. While this piece emphasizes the role of Western allopathic care, we at Tikkun believe that universal healthcare needs to include both allopathic and holistic healthcare. In this case, Western medicine is what was needed. We advocate for a Global Marshall Plan that would in part provide adequate healthcare throughout the world. — Cat J. Zavis]